The IUD Option: Stigma, Falsehoods, and Shaming
This post was written by Melanie Brewster and is cross-posted from Queereka.
This confession may come as a shock to some: I have never been in love with menstruation. The dread of a surprise attack, cramps, the discomfort of cotton wads crammed where no wads of cotton should be. While still respecting those who savor their bloody womanhood, I grew up wishing that I could do anything to turn off that monthly hell.
When I first started college I jumped on birth control pills, having always heard that they helped regulate menstruation, grow fabulous breasts, and clear up skin. It was obviously a win-win-win situation. Things looked even more promising when after a few years I learned that women could actually take birth control continuously (skipping the placebo pills) to avoid periods completely. Initially, I was a little concerned about the amount of hormones that would be pumped through my body, without giving it a “break” during the sugar pill week, but it seemed worth the risks. At that time, and still now, studies are somewhat inconclusive about links between cancers and hormonal birth control – it may serve as a protective factor against endometrial carcinoma and ovarian cancer, yet mildly increase risks for breast and cervical cancers. That said, every time I have gone to the gynecologist since I was 18, I have always asked about lower doses of birth control and am currently taking Avaine – levonorgestrel and ethinyl estradiol, 0.10 mg/0.02 mg tablets – which is about as “low as you can go” for pills. This equates to over a decade of asking for different treatment options from doctors in Florida, Utah, and New York.
Throughout the years, I heard tiny peeps about intrauterine devices (IUDs) as alternate methods of birth control. These peeps were mostly from anarcho-feminist friends, whose willingness to research new contraceptives, pop in Mooncups, and rock unkempt armpits always managed to intimidate and inspire. One friend tried an IUD and, while she loved it, it triggered lactation – something that no 23-year-old childfree riot grrl wants to deal with. This was the last I heard about IUDs for many years.
* * *
Forgive me for the wide-eyed awe, but you can imagine my surprise when, upon joining a support group for skeptic women runners, I learned that many women use IUDs. And, almost 80% of hormonal IUD (like Minera) users experience complete amenorrhoea when using them. No more periods! After doing more reading, this time informed by MEDLINE and Google Scholar searches rather than Facebook posts, I learned that because women don’t have to remember to take a pill at a certain time every day, failure rates for IUDs are stunningly lower than with oral contraceptives. This makes IUDs particularly attractive for adolescent and young women who are certainly not interested in having kids. Not only are these completely removable devices more effective than having your tubes tied, they can be removed anytime and last 3 to 5 to 10 years (depending on your needs). But, the shocker for me was that they use significantly less hormones than oral contraceptives. Despite my decade of pleas for lower doses of chemicals in my body, not one of the 8+ doctors I saw ever recommended IUDs. I didn’t understand why I hadn’t heard more about this option. I mean, I’m a professor, I specialized in sexuality and gender issues during my doctoral studies, I support Planned Parenthood, I read Jezebel! Surely it wasn’t just me being oblivious?
I was sold. Between the high likelihood of amenorrhea, lower dose of hormones, and ability to stop taking a pill every day for five years, an IUD sounded like a fantastic option. Nearly giddy, I scheduled my yearly appointment, thrilled to speak more about this option with a doctor and prepared to finally go off oral contraceptives.
* * *
Now, it should be noted that I don’t live in the middle-of-nowhere Midwest or a single-stoplight Southern town. My private women’s health clinic is in Manhattan, New York City, one of the primary hotbeds of liberal thought, 3rd wave feminism, and freethinkers. The morning of my appointment, I walked through Central Park on the way to the Upper East Side, mentally recapping all the facts I had recently learned about IUDs and lazily planning what to grab for lunch later. So, you can imagine my shock during the too-crazy-to-be-untrue scenario that followed.
I am taken back to my examination room by a young woman who is currently in medical school. She is way younger than me, but I put my ego aside and feet in the stirrups so she can do the exam. The largest wall in the room is taken up by a Renaissance-style painting of a maiden with long chestnut hair, horizontally collapsed by the side of a body of water, eyes unfocused. Not the most soothing image by which to undress. While applying KY to her gloved fingers, the medical student asks me if there is anything that I’d like to discuss during my visit. I bring up IUDs. Her young brow furrows and she asks me a number of pointed questions about my plans for childbearing. I tell her “as a young tenure-track professor at an ivy league school, there is no way in hell that I would even consider having a kid for at least five years. But honestly, I don’t think that I want them at all.” Seemed like a reasonable response to me.
She then asks me more questions about why I would ever want to get off of birth control pills. I explain, “having a period is annoying, I hate the amount of hormones I am putting into my body, and having to remember to take a pill everyday at the same time is tedious. Hormonal IUDs may solve all of these issues.”
Head tilted to one side, nose scrunched, she slowly tells me, “you will be hard-pressed to find a doctor in private practice in New York that would do that for you.”
“Huh?”
“IUDs are only implanted in women who have already had babies. Otherwise, the uterus is too tight. I strongly recommend against it. You can talk to the doctor about it, though.”
And, I did talk to the doctor, or rather, a RPA-C (registered and certified physician assistant); I suppose most people assume that anyone in a white lab coat is a doctor? She reiterated that I needed to give birth before they would ever implant an IUD, because my tiny pre-motherhood uterine opening could not handle such a foreign contraption, and added, that they cause severe cramping and infections. Generally, she made it sound as though implantation would trigger a life of uterine misery to which no young woman sound of mind would ever agree.
To be fair, there was a time, in the 1970s, when one particular brand of IUD, “the Shield,” was horrifically imperfect. Specifically, excessive bleeding, pain during sex, and abdominal discomfort were common side effects. There were also the more severe consequences such as pelvic inflammatory disease (PID) and higher failure rates than anticipated (and in turn, pregnancies with spontaneous septic abortions). Some women with extreme PID had to receive hysterectomies or were rendered infertile by scar tissue on their fallopian tubes. Lawsuits and panic ensued, and the market for IUDs in the U.S. tanked.
However, most brands of IUDs, even the early models from the 1970s, were completely safe. Modern IUDs are durable, safe, and effective but have not become the go-to method of birth control in the U.S. This is because most doctors trained after the aforementioned PID panic of the 1970s were never taught the truth about IUDs, or how to properly insert them. Thirteen years ago, the FDA cleared hormonal IUDs, such as Mirena, for sale in the U.S., however, broad support for IUDs is still lacking amongst many older doctors.
But, it is important to keep in mind that, similar to the medical student with whom I first interacted, the RPA-C was also very young. I point this out not to be ageist, but because it horrifies me that both women were espousing myths about IUDs generated from hysteria in the 1970s, when they are either currently in school or graduated in recent years. Almost too stunned to react to their lack of knowledge, I internally questioned where the hell these women had received their medical training.
Beyond surprise, I also felt disempowered. I came to their clinic after extensively educating myself about reproductive health options, yet was still made to feel that I was ignorant and misinformed about IUDs. To add salt to the wound, the RPA-C looked at me, and with mild condescension and the tone of a conservative Fox News anchor added, “I mean, if you are really set on doing this – I still think it’s a bad idea – but Planned Parenthood may do it.”
* * *
What? Really? A young woman who is trained as a women’s health professional is discounting safe and effective methods of birth control and bashing Planned Parenthood in the same sentence. Her comment subtly set up a dynamic that only overly progressive, publicly funded, and uninformed clinicians, such as those at Planned Parenthood, would ever be “so irresponsible” as to insert an IUD. No private doctor would take such a silly risk. Again, this is in New York City. If a women’s health center in Manhattan refuses to discuss IUD implantation, I now understand why I didn’t hear anything about this option when I lived in the south or Utah. Upon scouring the internet and women’s health message boards, I’ve stumbled across tons of stories from patients across the U.S. who have had similar interactions with doctors, nurses, and physician assistants.
To reiterate the facts: since 1998, studies have affirmed the safety of IUDs and assert that they are cost effective and highly efficacious forms of contraception for most women. Pointedly, an official statement by the ruling body of women’s health, The American College of Obstetricians and Gynecologists, in October 2012 decreed that IUDs were safe and appropriate for women, and adolescent girls (to be totally clear, even those who haven’t yet popped out a baby). Yet, here’s where it gets crazy: 41% of women in China use IUDs, 27% of Norwegian women, but less than 9% of women in the U.S. use them; a rate that is significantly lower than those in any other developed country.
For a nation that prides itself on medical advancements, it’s time that we bring women’s healthcare out of the disco-days of the 1970s. Doctors in the U.S. need to start listening to the FDA and American College of OB-GYNs and educating future generations of medical professionals about IUDs. But most importantly, medical professionals at all levels need to stop perpetuating myths about these very real, very important contraceptive options, and patients need to start calling bullshit when they hear such myths conveyed. I, for one, will be sending a care package filled with journal articles to my private women’s health center in Manhattan, along with a note explaining why I will no longer be their patient.





That’s really shitty of them. I was worried about something like that happening when I got my IUD (Mirena) in February. I’m 22 (I was 21 at the time), never been pregnant, and I’d been on the pill for a few years and I decided that an IUD was a better option. When the contraceptive mandate went into effect, I immediately made an appointment at a gynecology office in town (that town being Tallahassee, not the most liberal place in the country). I went in and had a check up and told the doctor what I wanted. She talked about it briefly and gave me a pamphlet about Mirena and told me to set up and appointment as soon as I got my next period. A couple weeks later I went back and she put it in, no problem (although it did hurt quite a bit). It’s been pretty great. There was a period of bleeding (kind of like spotting) for the first month, but now that’s stopped and I haven’t had a period since.
That is great to read. Women seem to adore Minera, and it’s wonderful to hear that not everyone has a “you should have a kid first” shaming experience!
Though the IUD has been a Godsend (so to speak) for a few people I know, it was a nightmare of epic proportions more often than not among my circle in the last few years. I’m told that having it implanted was an 11 out of 10 on the pain scale, with further cramping so bad that an eager would-be breeder had serious second thoughts about wanting to ever give birth. Not to mention bleeding heavily for three months straight before being able to get it out. I was too horrified in the first place at letting anything be shoved through my cervix to ever try it and am a happy long-time customer of the b.c. shot.
While having more options is great, I’m appalled at how heavily OB/GYNs are pushing the IUD lately and how simple they say it is even for nulliparous women. It’s really not a universally good choice for everyone, and providers seem to gloss over the horrors of common side effects.
People’s experiences of course vary but I didn’t find the implanting to be that painful. It certainly hurt and wasn’t much fun but not anything some ibuprofen and a hot pack on my belly for the afternoon didn’t solve. I had much worse side effects from the depo provera shot that I was on for many years before getting my IUD, mainly horrible mood swings the first week after each shot from the increase in hormones. People vary in how they respond to different birth control.
I have to say I really love my IUD and I’m glad to have an option that doesn’t mess with my moods or sex drive the way stronger hormonal birth control did (and gets rid of my F-ing period which I really hate and never want to experience again). It’s not for everyone but it’ an option more people should know about and I think the reason it seems to be getting pushed more is that fears around them have decreased. Apparently not enough based on Malanie’s experience.
Noadi, I think we’ve had similar experiences – Depo for me was an absolute nightmare, a solid three months of ridiculous mood swings and generally being a crying wreck. I loathed every second of it, and there’s nothing you can do to stop it. I liked implanon on well enough (the worst bit there is the anaesthetic), but wanted to move away from hormonal birth control – it messed with my moods too much. IUD insertion wasn’t fun, but tbh, I’ve had worse period pains. Apparently there’s a degree of skill on the part of the inserter that can make it more or less painful – I wanted to try a new Dutch design that’s meant to be better for nulliparous women, but my GP said she wasn’t comfortable with her skill at inserting them yet.
The Mirena has been great for me. Installation not exactly painful, but unpleasant, and made me feel a bit shaky afterwards for a while, but really no big deal for me. No periods (occasional spotting when I would otherwise be having my period). I am completely happy with it.
I think I tried to find out about getting an IUD before I’d been pregnant, and am fairly sure I was discouraged. I do know that I inquired about long term birth control without having to take a pill every day, and was led to believe there was no such option for me.
Then, while in hospital after giving birth, a doctor recommended an IUD and wrote me a prescription. So easy. It should have been easy for me during my long pre-pregnancy years of adulthood too.
I have had a Paragard IUD for several years. I am 40 years old with no children. I live in Florida. I was interested in birth control without hormonal effects like weight gain. My gynecologist mentioned the Paragard IUD easily with no reservations about my uterus size, but did say there would be cramping and spotting for a week or so. The implant took about 5 minutes, and I did have moderate cramping and spotting for about 7 days. Since then it has been the best decision of my life. It was even covered by my insurance. I had no idea that other people were having problems getting an IUD. I hope my experience helps others.
This post – http://freethoughtblogs.com/lousycanuck/2012/11/24/getting-a-mirena-iud/ – definitely made me think that some providers are downplaying the pain of implantation in their reigns of IUD evangelizing. But, seems like a few ibuprofen and half-day of work will do the trick for many women.
I’ve had Paraguard for four years now. I got it at age 21 without ever having been pregnant, let alone given birth, and at Planned Parenthood. It definitely meant a day off work and a lot of ibuprofen (and wine. and maybe some green stuff) but it was worth the trade-off for a decade of no babbies for me.
In my experience (been on and off BC for over 17 years…geez) OB/GYNs push their patients for any BC option that isn’t barrier-based. I’ve never been offered an IUD, but had the pill pushed on my many times despite complaints of serious side effects. Never once has a doctor suggested a diaphram in though. I even had a doctor at one point tell me, angrily, that I was definitely going to get pregnant because I decided to stop taking the pill for a while and rely on condoms.
I was nearly 30 in a long term (>5 years) monogamous relationship and had a good job. I informed her I was perfectly capable of preventing pregnancy or choosing to get pregnant if that’s what I wanted. More than 5 years later and I’ve still managed to not be pregnant. My sister in law had 2 children and wanted a tubal, the doctor tried to talk her out of it because she “was so young and might want more…” Similar story from my sister too.
I’ve long felt that doctors both underestimate women’s ability to make informed decisions about their reproduction and women’s own reporting of side effects/experiences with birth control. I think it’s a side-effect of the general attitude that women can’t be trusted to choose whether or not to have an abortion. I have felt that I am often treat like a child in this respect through glossing over side effects, ignoring reported side effects and pushing the doctor’s own prejudice on me. And clear it’s a fairly common experience.
That is so shitty! I am evangelical about Mirena, because my experience has been so positive. I’m in a similar situation to Melanie and instead of being rejected, I was told I was an ideal candidate! Of course, that was by a Planned Parenthood doctor – you know, one with decades of experience of being an OBGYN, so clearly she knew nothing and was just being irresponsible.
Installation was easy for me, though I had a bit of vasovagal reaction afterwards. Nothing a lie down and some juice couldn’t solve. And it has been magnificent to have almost no period. So much time and mental energy to devote to other things, not to mention the overall cost effectiveness of having a health-insurance covered birth control that means I don’t have to buy “feminine hygiene” products every month.
I know several women who have daughters with varying levels of developmental and cognitive delays. Several of them either have their daughters implanted with and IUD, or are planning to do so when the time comes. I had not heard that the new IUDs can be implanted in a nulliparous woman, so I was surprised to hear this. However, as these young women may be unable to care for hygiene needs, especially menstruation, I was impressed that so many doctors and OB/GYNs know and inform patients about these choices. It is also sad but true that sexual victimization of cognitively delayed women is prevalent, and and IUD can prevent an uninteded pregnancy.
I always wanted one, and I’ve just recently scheduled an appointment to get it. Honestly, I’ve been dreading talking to my doc about it ever since I started researching the issue and stumbling upon these kind of posts. Thankfully, the only thing she mentioned besides pain during the procedure, was that the aftermath of getting an infection while having an IUD can be more severe, so she wanted to know if I have a long-term trusted partner.
She works in a private clinic in the Midwest area, so there’s hope, I guess.
I love my Paraguard IUD. It doesn’t stop your periods (being non-hormonal) but I’m breastfeeding, so I don’t have those anyway, and probably won’t for a while. I will say that it hurt not at all going in, like zero, presumably because I had it implanted 12 weeks after giving birth. I’ve had no pain or side effects at all so far. So in that sense, it may be a somewhat better choice for women who have had children (recently!) than for those who haven’t.
In my post-natal condition, I was actually pushed toward Mirena. (The options for birth control are much more limited for breastfeeding women anyway.) My doctor reported that women loved the effects it had on their cycles, whereas Paraguard has the reputation of making them somwhat more unpleasant. I chose the non-hormonal option anyway for a variet of reasons.
I was rather surprised that no previous doctor had ever recommended IUDs to me before, so I guess that’s anecdotal evidence that they still aren’t being suggested for nulliparous women. I think doctors are just still a little nervous because there is some evidence that if you haven’t been pregnant, you’re more likely to have some pain or complications. But “more likely” is not “likely” in an absolute sense, and the research I did agrees with your conclusions — IUDs, hormonal or not, are safe an effective whether or not you’ve had kids, and are much better option than hormonal birth control pills or injections for many if not most women.
I will say that I *was* actively discouraged from using a diaphragm, though, when I brought it up as another non-hormonal option. I was told “hardly anyone uses those any more”!
Here’s an excellent article on whether an IUD hurts or not by Dr. Jen Gunter. She is a gynecologist that writes about women’s health issues with some science thrown in:
http://drjengunter.wordpress.com/2013/06/22/is-an-iud-painful-if-so-how-can-i-reduce-the-pain/
Ohhh, great find!
The real problem is a false sense of choice. Even after two kids, I was denied the right to have my tubes tied because both of the major hospitals in my area are run by catholic organizations. The only time they allow a woman to have a tubal is after meeting with the board of directors and showing that it is a truly life or death circumstance.
I tried after my first child to get an IUD and my doctor told me that he could refer me to OACAC or Planned Parenthood, because he didn’t believe in them.
There’s no doubt that science is affording us a lot of options, but finding a doctor who is willing or able to provide all of the options is becoming harder and harder. Especially here in the bible belt.
It amazes me that stuff like this still happens.
A friend’s mom almost died in the late 70s due to complications to a pregnancy with twins. She was very young, couldn’t support her family and almost died, but was denied a tubal ligation because she “was so young.” It wasn’t until the second pregnancy almost killed her (surprise still could handle it) that the doctor agreed.
We have a very long way to go.
It really is amazing. My first doctor openly told me after I had my oldest daughter that he was catholic and would prefer to not even give me pills. Luckily, he found it irresponsible to not at least give me that much. My second doctor would have gladly given me a tubal, but didn’t have access to a hospital who would allow it to happen. Even though I was having a cesarean, so it could have all been done in the same surgery. At least he was willing, but this is the problem with catholic run healthcare.
It’s really great to read that there are women who hate their periods as much as I do. I got a hormonal implant about 4 years ago and love it so much. My periods completely stopped (no period in 4 years, yay!) yet I’ve had so many women tell me that they like their periods and don’t want to stop them as it makes them feel ‘cleaned out’!. I’d take not having to buy tampons, no period pains and not having to remember when I’m due on (something I was never able to do) over feeling ‘cleaned out’ any day.
The implant doesn’t hurt as it’s done under a local anaesthetic. It has to be changed every two years (I’m currently arranging for the second one to be replaced) but I’d really recommend looking into them. I live in the UK and it’s free so I can’t say whether they’re more expensive than IUDs (I have no idea how the pricing of different contraceptives work in the US) but I’ve had friends complain about the pain of IUD fitting while I barely remember getting my implant changed, let alone feeling any pain.
As an aside, I remember as a women in my twenties trying to get a repeat prescription for the pill. The doctor asked me why I wanted it and my first response was ‘control’. Apparently that wasn’t good enough and I had to remember that I used to have really bad period pain and emphasise how bad they were before she’d give me the prescription. It still haunts me and I find myself preparing for grillings when I come to get new prescriptions, though I’ve not had any problems since. It just completely threw me that having control over my body wasn’t a good enough reason to take the pill! (And it was a female doctor!).
To be fair to the health care professionals, the FDA prescribing information (http://www.accessdata.fda.gov/drugsatfda_docs/label/2009/021225s027lbl.pdf) specifically recommends Mirena for women who have had at least one child. Delving deeper, we can see that the study initially used for FDA approval in 2000 was only conducted on women who had previously been pregnant. So, there is a scientific basis for hesitancy with this product. It probably is safe for most women, but that’s really not reflected well in the prescribing documentation.
I suspect this incident has less to do with stigma or shaming than it does with risk-assessment by two people who feel like they have to do everything by the book and with extra caution. Consider this: A medical student has very little real-world experience and an RPA-C is operating in an environment where her mistakes are legally the responsibility of the physician who oversees her. So, although many docs may be comfortable saying “This is safe, let’s do it,” a PA is thinking “If I do something the FDA thinks is unsafe and something goes wrong, my boss could go to jail.”
So sorry to hear about your terrible experience and misinformation. Even if the medical student who saw you was giving you all of the information to the best of her knowledge, it sounds like she needed a much better attitude.
I got a Mirena last November. I had been contemplating it for a year or so, and when I asked about it, both the doctor and NP I saw told me that the recommendation against IUDs for women who had not had children was simply because insertion would be more difficult and painful–no other risks. I put it off for awhile, but the benefits eventually outweighed the costs.
My insertion experience was terrible, actually. I wasn’t reminded that I needed to take ibuprofen BEFORE the procedure, and after the fact it was too late for it to work right away. The procedure itself wasn’t awful and was over quickly, but I had terrible cramps immediately following and had to lie in the room for awhile after. I went by myself, which was also a mistake, especially when it was clear that they wanted me to leave the room. The receptionist called a cab for me, but I waited outside and it never showed up, so I ended up walking to a train (the walk was actually the first thing that made my cramps feel better). I went back a month later for a follow-up, and it the doctor couldn’t find the end of the string, so she made me go get an ultrasound to make sure the Mirena was positioned correctly. Turns out she doesn’t do these insertions often–would have been good to know that beforehand so I could have requested someone else. This is probably my biggest recommendation (after remembering to take pain meds in advance): you want someone comfortable with the technology doing the insertion.
Since then, it’s been pretty great. My periods haven’t stopped (yet?) but they are much, much lighter. They’re not regular right now–I know it’s coming because my breasts are sore for the week prior, and they last longer than my periods did on the Nuva Ring, but are so much lighter than they were before I ever went on BC. The end of the string seems to be curled up inside my uterus, so removal will be…less than ideal, but I’ve got more than four years to go before then.
Ahh, I posted on the Queereka article instead of here. My bad.
While I am annoyed by the lack of up-to-date information in the OBGYN community about this, I’m not at all shocked. The way that OBs in the US handle maternity care – from unnecessary interventions to lack of support for midwives/homebirth to a 33% Caesarean rate to low support for VBAC – has resulted in the US being rated #50 in the world for maternal mortality. (Source: http://www.huffingtonpost.com/2012/08/24/maternal-mortality-rate-infographic_n_1827427.html)
Ask skeptics, we all want evidenced-based care from out doctors. Evidence that vitamins actually work. Evidence that a drug is safe and effective. Evidence that the advice we’re being given is a result of the latest studied and research and not woo from the 1970?s. It is unfortunate and disturbing that so many doctors, who purport to be educated, fail to provide us with the best medical care due to ignorance and stubbornness.
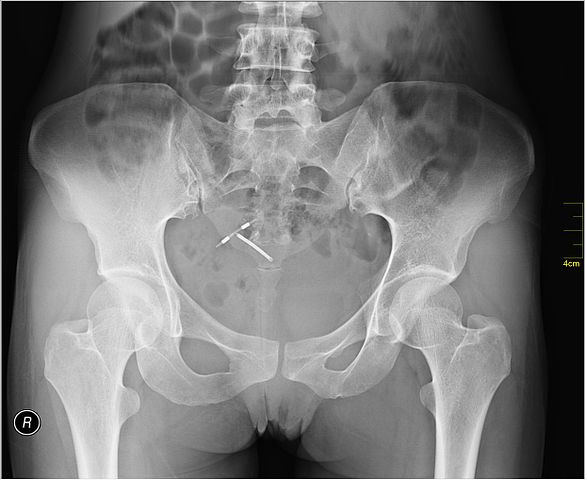
Side note: that X-ray shows an IUD (looks like Paragard) that has perforated and migrated out of the uterus.
On topic: for many women, IUDs are a wonderful thing. Statistically very few women have the experience Moniqa referenced above but it does happen. There are contraindications but not many.
I really lucked out on my experience with the IUD; and I didn’t even know I lucked out until after I already got it, because I only started hearing stories like this years after getting my own Mirena without any problem (but then, I did go straight to PP, not having had insurance). They informed me of all the possible problems (pain during insertion, cramps for a while after, high chance of complications from infections) but didn’t even say anything about how it’s only recommended for women who had already been pregnant.
The only thing I wish had been different is that the degree of worry about pain after insertion was backwards: I didn’t get any pain-med prescription the 1st time, and that’s when I did experience serious cramping; the 2nd time I got prescription-strength ibuprofen AND acetaminophen+codeine… and it turned out mostly unnecessary.
BTW, there’s one other way in which clinics discourage women from getting IUDs: a friend of mine was told it would cost $3000 to get an IUD (it cost me nothing the first time, $800 the second time).
I asked for a tubal ligation at 27, but my doctor wouldn’t do it because I was “too young” to make the decision to never have kids, but she suggested an IUD. It was a non-hormonal IUD and it was a little painful, but not too bad. I had it removed three years later and went back on the pill because I had a mental block about having a piece of metal inside me.
Five years ago I started taking the pill continuously because I didn’t see a need to have a period. I still don’t and I still don’t have one. I didn’t realize that a hormonal IUD would do the same thing. I plan to ask my doctor about it at my appointment in January. My birth control isn’t free under my health care plan until January because my health care plan was grandfathered in. :/
When I asked my doctor about non-hormonal birth control at the age of 27 Paraguard was the first thing she brought up. I’d never had a pregnancy, so she told me I was at greater risk of my uterus pushing it out (which it ended up doing twice before I gave up on the idea) but she was very honest about how effective they were, how quick and easy insertion and removal would be, and how small the risk of side effects was.
And, just for good measure I want to correct a typo:
“IUDs are only implanted in women who have already had babies. Otherwise, the uterus is too tight. I strongly recommend against it. You can talk to the doctor about it, though.”
That should read the CERVIX is too, tight. Whoops ;)
Manhattan doctors are assholes. Come to Brooklyn, my OB will hook you right up.
My understanding is that insertion is more difficult on a woman who has not given birth (and therefore more risky for the doctor and more painful for the patient), but an experienced OB should be able to do it.
Great article.
For those of you who can read French (or Italian, as that part of the site was translated), Dr Martin Winckler’s web site* contains a lot of information about contraception, including IUDs for women who haven’t had babies:
http://www.martinwinckler.com/spip.php?rubrique34
He also wrote a thorough book on contraception in 2001, “Contraceptions mode d’emploi”.
* That’s his pen name when writing novels. His real name is Dr Marc Zaffran
http://en.wikipedia.org/wiki/Martin_Winckler